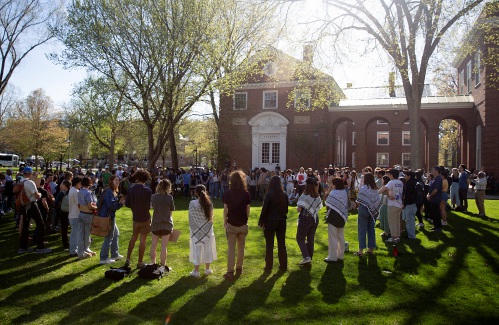
Dartmouth administration faces fierce criticism over protest arrests
HANOVER — Dartmouth President Sian Beilock and college administrators faced pointed criticism at a meeting with faculty on Monday regarding the arrest of 89 students, staff, faculty and community members by police in riot gear at a protest on the...

Local Roundup: Hartford tops Woodstock in close girls lacrosse contest
Editor’s note: To have your team’s results included in the Local Roundup, visit https://www.vnews.com/submit-a-score.Girls Lacrosse Hartford 11, Woodstock 7 Key players: Hartford — Audrey Rupp (six goals, one assist), Madi Barwood (three goals), Nella...
Most Read
 Dartmouth administration faces fierce criticism over protest arrests
Dartmouth administration faces fierce criticism over protest arrests
 Three vie for two Hanover Selectboard seats
Three vie for two Hanover Selectboard seats
 A Look Back: Upper Valley dining scene changes with the times
A Look Back: Upper Valley dining scene changes with the times
 Norwich author and educator sees schools as a reflection of communities
Norwich author and educator sees schools as a reflection of communities
Editors Picks
 Norwich author and educator sees schools as a reflection of communities
Norwich author and educator sees schools as a reflection of communities
 Editorial: Response to campus protests only adds fuel to the fire
Editorial: Response to campus protests only adds fuel to the fire
 Kenyon: Dartmouth shows it has no patience for peaceful protest
Kenyon: Dartmouth shows it has no patience for peaceful protest
 Publisher’s note: Valley News launches updated online app
Publisher’s note: Valley News launches updated online app
Sports
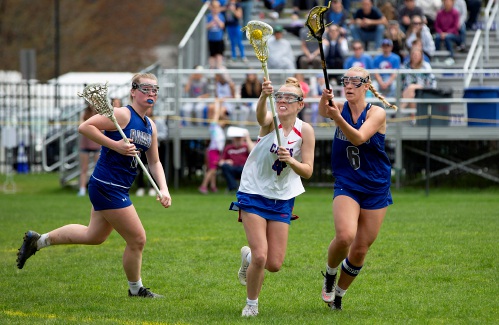
Hurricanes earn 10-9 victory over U-32 in girls lacrosse
WHITE RIVER JUNCTION — The pass was perfect, a classic backdoor feed that arced from Paisley Danaher to Madison Barwood and resulted in the winning goal Saturday for the undefeated Hartford High girls lacrosse team.The strike lifted the host...
 Stevens, Newport baseball split high-scoring games
Stevens, Newport baseball split high-scoring games
 Lebanon High senior comes to the aid of driver with health problem
Lebanon High senior comes to the aid of driver with health problem
 Oxbow softball at dynastic, dominant best
Oxbow softball at dynastic, dominant best
 Local Roundup: Lebanon wins big over Bow in boys tennis
Local Roundup: Lebanon wins big over Bow in boys tennis
Opinion

Editorial: Chris Sununu’s moral vacuum
New Hampshire Gov. Chris Sununu’s conversion from “Never Trump” to “Ever Trump” occurred not on the road to Damascus but on the Republican Party’s road to perdition.On ABC News last Sunday, Sununu affirmed his intention to support Donald Trump for...
 Editorial: Gambling tarnishes America’s sporting life
Editorial: Gambling tarnishes America’s sporting life
 By the Way: A white nationalist’s many mistruths
By the Way: A white nationalist’s many mistruths
 Column: The age-old question of what to read
Column: The age-old question of what to read
 Editorial: Transparency wins in NH Supreme Court ruling
Editorial: Transparency wins in NH Supreme Court ruling

Photos

Pampered pup
 Eyes and ears
Eyes and ears
 Afternoon outing in Norwich
Afternoon outing in Norwich
 In the garden
In the garden
 Spring cleanup in Lebanon
Spring cleanup in Lebanon
Arts & Life

A Look Back: Upper Valley dining scene changes with the times
Before franchised fast food and corporate-owned restaurants hit the Upper Valley, there was a time when locally owned diners and a variety of family-run eating establishments flourished and produced many fond memories and much nostalgia. For at least...
 The future of fertilizer? Pee, says this Brattleboro institute
The future of fertilizer? Pee, says this Brattleboro institute
 Bald eagles are back, but great blue herons paid the price
Bald eagles are back, but great blue herons paid the price
Obituaries
 Barbara Mae Sprague
Barbara Mae Sprague
Lyme, NH - Barbara Mae Sprague (Hood), age 92, passed Tuesday, November 7, 2023. A graveside service for Barbara will be held on June 4th at 11 am at the Highland Cemetery (on High Street in Lyme, NH). Friends and family are welcome... remainder of obit for Barbara Mae Sprague
 Richard A. Pecor
Richard A. Pecor
Richard A. "Dick" Pecor, Jr. Canaan, NH - Richard A. "Dick" Pecor, Jr., 63, formerly of White River Junction, VT died at his home in Canaan, NH on Thursday, May 2, 2024. Dick was born July 9, 1960, in Burlington, VT to Richard and Carolyn ... remainder of obit for Richard A. Pecor
 Lyell Converse Smith Jr.
Lyell Converse Smith Jr.
Lyell Converse Jr. "Skip" Smith Orange, NH - Lyell Converse Smith Jr. known lovingly by all as "Skip" passed away on May 1st, 2024 at the VA hospital in White River Junction, VT after a brief illness. He served in the United States Army ... remainder of obit for Lyell Converse Smith Jr.
 Lawrence Swett
Lawrence Swett
Lawrence "Roger" Swett West Lebanon, NH - Lawrence "Roger" Swett, age 84, passed Friday, May 3, 2024. A full obituary will be published in an upcoming edition of the Valley News. Ricker Funeral Home of Lebanon, NH has been entrusted... remainder of obit for Lawrence Swett


 Hanover house added to New Hampshire Register of Historic Places
Hanover house added to New Hampshire Register of Historic Places
 After reaching agreement with Middlebury College, student protesters take down encampment
After reaching agreement with Middlebury College, student protesters take down encampment
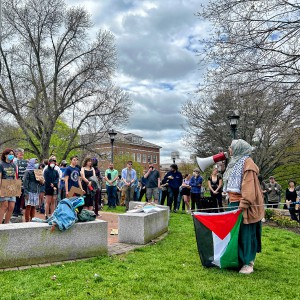 UNH faculty and students call on university police chief to resign following his alleged assault on a student
UNH faculty and students call on university police chief to resign following his alleged assault on a student

 From dirt patch to a gateway garden, a Randolph volunteer cultivates community
From dirt patch to a gateway garden, a Randolph volunteer cultivates community  Out & About: Newport art center’s exhibition celebrates homes of all varieties
Out & About: Newport art center’s exhibition celebrates homes of all varieties