Upper Valley residents among advocates for NH aid-in-dying bill

Susan Gillotti, of Hanover, N.H., has become an advocate for the proposed New Hampshire aid-in-dying bill. While living in Vermont, Gillotti's husband, Al Gillotti was protected by its state law allowing terminally ill people to end their lives. Behind Gillotti is a portrait of her and her husband. (Valley News - Jennifer Hauck) Copyright Valley News. May not be reprinted or used online without permission. Send requests to permission@vnews.com. Valley News – Jennifer Hauck
| Published: 04-22-2024 7:31 PM |
HANOVER — Before she moved to Hanover, Susan Gillotti was hesitant.
“I said that I wanted to move a continuing care retirement community in New Hampshire, but I was really afraid of doing it because I’d lose my entitlement to medical aid in dying,” said Gillotti, 85, who moved from Norwich to Kendal at Hanover in October 2022.
Medical aid in dying was particularly important to her because her late husband of 56 years, Al, had used Vermont’s law in 2018 after being diagnosed with a terminal brain tumor.
“I will be forever grateful to my husband for giving me a day that is joyful to recall rather than painful,” Gillotti said. “His dying was so sweet, serene and peaceful. He was so relaxed about it.”
Now Gillotti is advocating for New Hampshire to pass its own medical aid in dying law. She is one of dozens of Upper Valley supporters who are hopeful that, after years of advocacy work, New Hampshire could be the next state to pass a “medical assistance in dying law.”
The proposed legislation, which originated in the New Hampshire House of Representatives with lead sponsor state Rep. Marjorie Smith, D-Durham, was approved by the House by a vote of 179-176, with bipartisan support in March.
While the bill’s passage in the House was encouraging, state Sen. Sue Prentiss, D-Lebanon, who is a supporter, but not a sponsor of the bill, cautioned that it will face a more difficult road in the state Senate.
A hearing before the Senate’s House and Human Services Committee is scheduled for 10 a.m. Wednesday in Room 103 at the New Hampshire Statehouse in Concord. There is also a streaming option available via YouTube: youtube.com/@NewHampshireSenate/streams.
Article continues after...
Yesterday's Most Read Articles
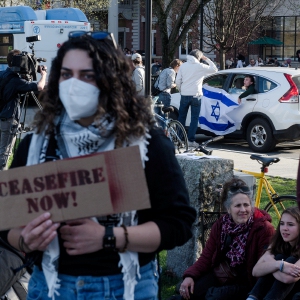 Dartmouth moves swiftly to stymie demonstration, leads to 90 arrests
Dartmouth moves swiftly to stymie demonstration, leads to 90 arrests
 Dartmouth graduate student-workers go on strike
Dartmouth graduate student-workers go on strike
 At Dartmouth, hundreds protest ongoing war in Gaza and express support for academic freedom
At Dartmouth, hundreds protest ongoing war in Gaza and express support for academic freedom
 Art Notes: City Center Ballet celebrates 25 years
Art Notes: City Center Ballet celebrates 25 years
“My read is that, unfortunately, it’s going to be tough,” said Prentiss, who is a member of the committee. “I’m not sure, it is my read — with the exception of a few Republicans — that they’re not going to be in favor of this. I have Democrat colleagues, very thoughtful ones, who are very on the fence.”
State Sen. Ruth Ward, R-Stoddard, whose district includes the Upper Valley communities of Charlestown, Claremont, Croydon, Newport, Sunapee and Unity, strongly opposes the bill.
“We are trying very hard and have prevention of suicide bill to help people not to get to that point,” Ward said. “We spend a lot of time and effort on that. Now we have a bill where we actually encourage legal suicide, and I just can’t support it.”
She is worried that, even though people would need a terminal illness to be able to qualify for medical aid in dying, “it still opens up the door.”
She is also worried that family members might pressure elderly family members to use it toward the end of their life.
“I just think it’s the wrong thing to do,” Ward said. “I think at some point someone is going to use it to their advantage.”
Prentiss herself supports it, in part, because she is a big believer in allowing people to make their own choices about their medical decisions.
“This is the closest that we’ve come in a long time and we have an opportunity here to allow folks who are terminally ill (to make decisions) about how they want the end of their life to take place,” she said. “I think that’s a really personal decision and I think we should let them make that with their doctor.”
Prentiss emphasized that the proposal also is narrowly tailored. The bill calls for allowing health care providers to prescribe medications to patients with terminal illnesses who have a projected six months or less to live. Patients would have to undergo a mental competency exam and make the request to their physicians, among other qualifications. Health care providers — including pharmacists — could decline to fill the prescriptions if it interferes with their personal beliefs. Patients must also be able to take the medications themselves.
Cappy Nunlist, a retired attorney who lives in Lebanon and has been a longtime advocate for the state to adopt medical aid in dying, said that she has noticed a shift in public perception over the last few years.
“More and more people have dealt with mostly parents or spouses or siblings who have had life-ending diseases and other things, and it has been traumatic for the entire family,” said Nunlist, who has helped organize letter writing campaigns to lawmakers to encourage them to support New Hampshire’s bill. “They look at this loved one and say this should not be happening. They should not have to go through this pain.”
Gillotti, too, said that she’s noticed a difference in the way people talk about end-of-life care and how they want their deaths to be. She makes an effort to engage people in those conversations and has found that people have become more receptive to talking about it.
“Most everyone I know has tossed and turned at night being terrified at the process of dying,” Gillotti said. “They know that there’s a way for it to be serene and gentle and that’s what they want.”
If New Hampshire passes the bill it would join its neighbors who have similar laws.
Vermont’s Medical Aid in Dying Act was passed in 2013 and Maine’s Death With Dignity Act became law in 2019.
New Hampshire lawmakers have had the ability to look to their neighbors to see how those laws have played out, Prentiss said.
Dr. Brian Lombardo is a family medicine provider at Alice Peck Day Memorial Hospital in Lebanon, where he also serves as the medical director for primary care.
He also is licensed to provide care in Vermont.
“I think it’s quite honestly ... very unfortunate that patients know that this opportunity is available across the river, but they can’t pursue this option with their longstanding care providers in the state of New Hampshire,” Lombardo said.
Around six years ago, Lombardo was treating a patient in Vermont who had terminal cancer. He remembered the state’s medical aid in dying act and mentioned to his patient that it was one of his options.
“That was what prompted me to learn about the details of the process and made me realize how important it was for some people to have that as a tool,” Lombardo said. In the years since, Lombardo has helped around 15 patients in Vermont, including four from out of state, who were able to take advantage of Vermont’s law after the state became the first to expand eligibility to those who reside elsewhere last spring.
Expanded eligibility requires people to establish care in Vermont. In order for New Hampshire residents to use Vermont’s law, they have to establish care with a new medical provider “during a very critical junction in their medical journey,” Lombardo said. “It’s a very emotional and sensitive time.”
Most of Lombardo’s patients who have used medical aid in dying have either had experience in their professional lives with end-of-life care or personal experiences with severe pain associated with their illness.
Some, who have been near death before with their disease “have said ‘I just do not want to go there.’ They know what the suffering can be like and they have absolutely no interest in waiting for the disease process to control their death,” Lombardo said. “They want some semblance of control over an otherwise uncontrollable process.”
While hospice care does aim to make patients comfortable at the end of their lives, primarily through pain management, sometimes it isn’t enough. Lombardo’s first patient to consider medical aid in dying died before he could medically end his life. Still, knowing he had the option gave him comfort.
“Even just starting the process gives people relief,” Lombardo said. “This is another tool I think should be available to patients if they think it is what is right for them.”
Liz Sauchelli can be reached at esauchelli@vnews.com or 603-727-3221.

 Colby-Sawyer names interim president
Colby-Sawyer names interim president