Health workers testify of abuse
| Published: 02-07-2023 2:59 PM |
Smacked in the face. Punched and choked. Kicked in the stomach so hard you throw up.
Nurses, doctors and administrators from hospitals around Vermont provided those examples of violence — from just the past week — to lawmakers last Wednesday. One after another, in often tearful testimony, the direct care providers also described their most traumatizing experiences from the last few years.
“I have been spit at, kicked, had my hair pulled, been sexually harassed, had my life threatened,” said Jill Maynard, director of emergency nursing at Southwestern Vermont Medical Center in Bennington, Vt. In one case, she said, the patient who threatened her began stalking her in the community and near her family’s home.
During a joint session of the Senate Judiciary and Health and Welfare committees, 10 witnesses organized by the Vermont Association of Hospitals and Health Systems urged legislators to support S.26. The new bill would add three clauses specific to health care workers and health care facilities to Rule 3 of the Vermont Rules of Criminal Procedure, which governs when law enforcement officers can arrest someone without a warrant.
Health care workers experience the large majority of non-fatal illnesses and injuries from workplace violence nationwide — 73% in 2018, according to the U.S. Bureau of Labor Statistics. Many hospitals and other health care facilities in Vermont and across the country try to counter the risk by putting staff through de-escalation training, setting aside quiet spaces for decompression and creating crisis response teams that include mental health workers and security personnel.
But, all the witnesses said, in the past few years, the frequency of violent incidents and their intensity have gotten much worse. As hospitals, and long-term facilities that they discharge to, struggled with the COVID-19 pandemic and extreme staffing challenges, patients became frustrated waiting longer for care and institutional systems for coping began to fray.
Currently, in many cases, police officers will come to a hospital in response to a report of violence but will only issue a written citation, witnesses said. As a result, the person lashing out or making threats, who is sometimes a patient, other times a family member, often remains in the hospital after an incident. That sometimes leads to further violence.
In one case, a patient threw a urinal at a nurse over a nighttime shift, hitting her, and was cited but not arrested, said Alison Davis, medical director of the emergency department at Rutland Regional Hospital. He continued to taunt and threaten staff throughout the following day and later punched a different staff member, breaking her nose so severely it required two surgeries to repair, she said.
Article continues after...
Yesterday's Most Read Articles
 Crowd turns out to honor late Ascutney Fire Chief Darrin Spaulding
Crowd turns out to honor late Ascutney Fire Chief Darrin Spaulding
 Former principal of South Royalton School released from prison
Former principal of South Royalton School released from prison
 Pick a sport and Pete DePalo’s has probably officiated it over the past 40-plus years
Pick a sport and Pete DePalo’s has probably officiated it over the past 40-plus years
 Upper Valley residents among advocates for NH aid-in-dying bill
Upper Valley residents among advocates for NH aid-in-dying bill
 NH man convicted of killing daughter, 5, ordered to be at sentencing after skipping trial
NH man convicted of killing daughter, 5, ordered to be at sentencing after skipping trial
“One of the most disheartening statements I hear from my staff when assaults happen is, ‘No one is going to do anything,’ ” Davis said. “I hope that I can go back to them and say that our legislature is going to help.”
Vermont law currently allows law enforcement officers to make arrests without warrants in the situations described on Wednesday, said several legal experts who testified Thursday morning before the Senate Judiciary Committee.
“It seems like it really is a matter of discretion on the ground for the officer of how he or she wishes to go forward after speaking to the parties, and perhaps the state’s attorney,” said Chief Superior Judge Thomas Zonay.
Senate Judiciary Chair Sen. Dick Sears, D-Bennington, the bill’s primary sponsor, acknowledged that might be true. “Whether or not they can already do it, you probably are correct, but they aren’t doing it,” he said.
The goal of the legislation is to emphasize as a matter of policy the importance of responding to violence against health care workers, he said. Similar language in Rule 3 calls out cases of violence against family or household members and against vulnerable adults as particularly sensitive situations and allows law enforcement to make an arrest quickly.
Tim Lueders-Dumont, an attorney for the Vermont Department of State’s Attorneys and Sheriffs, agreed that the special language around domestic violence made a practical difference, if not a legal one.
“These are typically fast-moving situations,” he said. “You don’t have to fuss through the facts too much to figure out how to help that law enforcement officer when they are asking, ‘What can I do right now?’ ”
However, he added, in most of the cases, the person arrested would likely not be held but simply booked and released.
“I am less concerned about the outcome of what happens,” Sears said. “It is about the removal from the emergency room of the person who is creating the disturbance.”
More training for law enforcement on responding to these situations would be needed for the new bill to have any impact, said Defender General Matthew Valerio. Providing training about what is possible under current law would have the same effect, he suggested.
“To me, you are dealing with a law enforcement implementation issue by changing the law,” he said.
But, he said, “it’s not a legal problem at all. It’s a mental health issue, a drug abuse issue, a poverty issue, issues of despair and the like. That is not going to be dealt with with Rule 3.”
Sen. Tanya Vyhovsky, P/D Essex, agreed.
“To me, this is a symptom of a need to invest in our communities,” she said. “I support anything we can do to keep our health care workers safe, of course, but I don’t think we are getting anywhere close to the root of this problem.”
Those taking care of patients say that these more abstract issues mean less than just doing something to address a situation that is exacerbating staff departures and limiting recruiting.
Nursing staff are leaving at an alarming rate due to the increasing violence, said Danielle Boudro, a registered nurse and director of the progressive care unit at Northwestern Medical Center in St. Albans, Vt.
That concern was echoed by Ben Smith, a doctor and medical director of the emergency department at Central Vermont Medical Center in Berlin, Vt. “We are not a bottomless resource that can absorb all this forever,” he said.
For caregivers, each violent episode has the potential to be career-ending and life-changing.
Nurses from University of Vermont Medical Center in Burlington and Mt. Ascutney Hospital in Windsor each described brutal physical attacks by patients in the emergency room in recent years. The grappling and punches left them with significant brain injuries, constant anxiety and, in the latter case, ongoing hearing loss.
Matthew Looft, a nurse at UVM Medical Center, is still on heightened alert 20 months later, he said. He is working with administrators in the network to increase mental health support for caregivers who have suffered trauma on the job.
Mark Sacco, emergency department manager at Mt. Ascutney Hospital, said that all or almost all of the providers on his night shift were seriously injured trying to subdue a teenager brought there by his parents. Three of the six no longer practice. He feels he probably should have retired. But after a torturous three-month recovery, he returned to assist his colleagues during the COVID-19 surge.
“Please take this baby step, I implore you,” Sacco said.

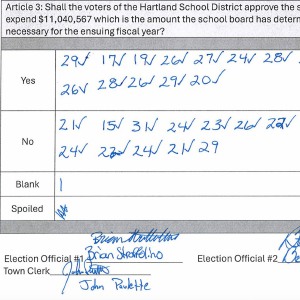 Hartland voters successfully petition for school budget revote
Hartland voters successfully petition for school budget revote